Reflux & Hiatal Hernias
REFLUX / HEARTBURN / GORD
Gastro-oesophageal reflux disease (GORD) is a very common condition which occurs when stomach acids leaks from the stomach and moves into the oesophagus (food pipe). This causes heartburn/indigestion and can eventually lead to damage to the lining of the oesophagus. It can affect anyone even children. It is usually treated with lifestyle changes (weight loss, smoking cessation, avoiding excessive alcohol, avoiding foods that trigger reflux ie. spicy foods) and medications to reduce the acidity of the stomach. If symptoms are severe, surgery may be an option to treat GORD.
Causes
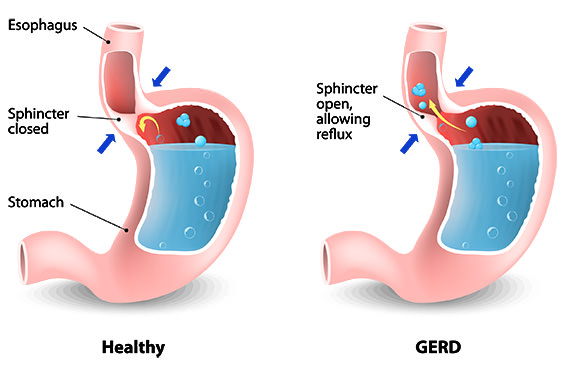
There is a natural barrier/valve (lower oesophageal sphincter) that prevents reflux between the stomach and the oesophagus. GORD occurs when there is dysfunction of this barrier. Things that can affect this barrier include:
– Hiatus Hernia: this occurs when part or all of the stomach migrates from its position in the abdominal cavity into the chest through the diaphragm. This disrupts the valve and allows acid to flow into the oesophagus.
– Oesophageal Dysmotility: normally the oesophagus propels food into the stomach in a progressive manner. When the oesophagus does not contract normally, this can lead to dysfunction of the lower oesophageal sphincter.
– Obesity / increased BMI: with increased weight, there is increased pressure in the abdominal cavity that leads to reflux. This increased pressure can also lead to a hiatus hernia forming.
Symptoms:
Reflux symptoms can be divided into typical symptoms or atypical symptoms.
Typical symptoms:
- Heartburn: a feeling of burning that rises up from the stomach
- Regurgitation: stomach acids comes back up into the mouth causing an unpleasant, sour taste
- Pain when swallowing or difficulty swallowing
Atypical symptoms:
- Chest pain
- Cough
- Recurrent chest infections; pneumonia, asthma
- Hoarse voice
- Sinus problems / infections
- Ear pain
- Dry, sore throat
- Dental damage
- Halitosis (bad breath)
- Throat clearing
Tests:
– Upper endoscopy to look for a hiatus hernia and Barrett’s Oesophagus (damage to the oesophagus from reflux).
– Acid testings: 24hr pH studies where a thin tube is placed via the nostril into the stomach to test for acidity within the oesophagus and the stomach. This is usually ordered to confirm GORD.
– Manometry: pressure testing of the oesophagus is where a thin tube is temporarily placed via the nostril into the oesophagus to check for the motility of the oesophagus. This helps to guide the surgical management.
– Barium swallow: a test done in a radiology (X-Ray) department where a dye is swallowed and images taken to see the anatomy of the oesophagus and stomach. This may identify a hiatus hernia.
Diagnosis
GORD can be diagnosed based on your symptoms. If symptoms are atypical then the diagnosis is usually made after performing one or more of the above tests. Total Upper GI Surgery will ensure that you undergo appropriate investigations to allow you to make an informed decision regarding treatment.
HIATUS HERNIA
A hiatus hernia is where part or all of the stomach migrates from its normal position in the abdominal cavity, into the chest. This commonly causes reflux and can lead to more serious health problems depending on the amount of stomach that has migrated into the chest. Occasionally, patients can present where the stomach has twisted or folded on itself (gastric volvulus) and this is a surgical emergency and you should present to your nearest emergency department. If left alone, “giant hiatus hernias” can cause problems at an increasing rate of 1% per year.
Causes:
A hiatus hernia occurs when there is increased pressure in the abdominal cavity that pushes the stomach upwards. There are naturally attachments that keep the oesophagus and stomach attached to the diaphragm, when these weaken; a hiatus hernia is more likely to form.

Symptoms:
- Asymptomatic (no symptoms)
- Dysphagia (difficulty swallow)
- GORD/regurgitation
- Breathing problems
- Gastrointestinal bleeding
- Chest/abdominal pain due to gastric volvulus.
Tests:
- Upper endoscopy
- Barium swallow
- CT scan
Diagnosis
When the diagnosis of a hiatus hernia is made, the Total Upper GI Surgery team will discuss with you the relevant pros and cons of surgery versus a non-operative approach and help you come up with an informed decision that suits the symptoms that you may be experiencing.
OESOPHAGEAL MOTILITY DISORDER
The oesophagus (food pipe) usually functions to contract and propel food that has been ingested down to the stomach. Oesophageal motility disorder is any medical condition in which the oesophagus doesn’t work properly and can lead to an array of symptoms including difficulty swallowing, spasm type pain and regurgitation of food.
Causes
There are a number of well-described conditions that cause oesophageal dysmotility, some of which can have good results with surgery. Achalasia is one such condition in which there is a potential surgical treatment that can help to alleviate some of the symptoms encountered by patients.

Symptoms
- Anxiety
- Chest pain
- Difficulty swallowing
- Heartburn
- Recurrent chest infections
- Regurgitation
- Weight loss
Tests
- Upper endoscopy
- Barium swallow
- 24hr oesophageal pH testing (acid testing)
- Oesophageal manometry (pressure testing)
Diagnosis
If oesophageal dysmotility is suspected, Total Upper GI Surgery will arrange for the appropriate testing to be performed to ensure that your condition is correctly diagnosed and the appropriate treatment offered. Certain medical conditions will respond well to surgery where as other conditions may not. Total Upper GI Surgery will ensure that you have the correct diagnosis prior to discussing treatment options.


